Managing the denial management workflow in medical billing is a very important part that ensures healthcare providers get paid for their services. We know that the denial process can be very frustrating for physicians, clinics, and hospitals. Research shows that healthcare practices cost 5-10% of their total revenue annually due to the complexity and inefficiency of healthcare insurance and coding.
So, understanding of the denial lifecycle isn’t enough for recovering the rejected claims. You need an efficient denial management workflow in place. Because only it can help you reduce revenue loss and improve cash flow.
In this article, we’ll walk you through the step-by-step process of denial management in medical billing. Further, you‘ll also know how it works and why it’s important. So, if you are a physician, clinic, or healthcare facility, the understanding of denial management is key.
What is Denial management?
Before we start discussing the detailed steps, the most important thing is to understand what denial management is. It is a process of identifying, analyzing, and resolving insurance claim denials. During this, the reasons for the denied claim are first reviewed, and the denials are appealed. After that, all the billing codes and medical records are checked to confirm their accuracy.
And this management plays an important role in maintaining a healthy revenue cycle. But if a claim is denied, it can significantly delay reimbursement and can affect cash flow. Ultimately, it’ll lead to poor financial health for a healthcare provider. That’s why properly managing and resolving denials will increase the chances of claim approval. And it also reduces the need for costly appeals.
What Steps are involved in Denial management Workflow?
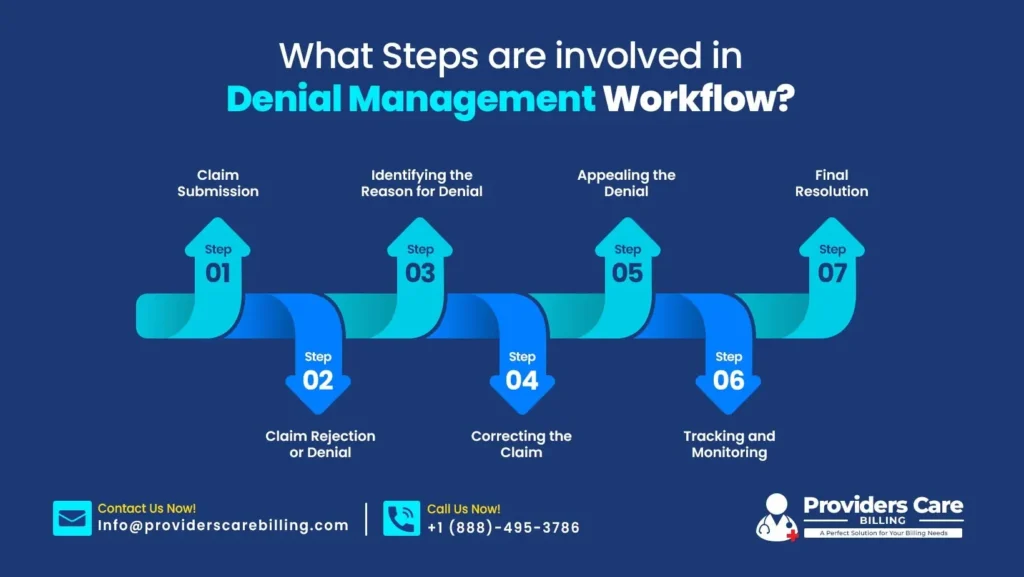
Step 1: Claim Submission
It is the first step of the denial management workflow. During this, all the information related to a patient, such as their medical records, diagnosis codes (ICD-10), procedure codes (CPT), and billing details, is gathered. Then submitted to the insurance company for payment.
So, if a claim isn’t submitted correctly, whether due to incorrect coding or missing information, it can lead to denied claims immediately. That’s why accuracy at this stage is considered most crucial.
And we, Providers Care Billing, LLC, with our years of experience, always make sure that claims submitted on behalf of our clients are 100% accurate. Because we deeply understand the intricacies of medical billing services.
Step 2: Claim Rejection or Denial
After submission, the insurance company will review the claim thoroughly. If everything is fine and in order, they will process it and will send reimbursement. But if they notice something wrong, the claim will either be rejected or denied. And this is what we call claim rejection.
Step 3: Identifying the Reason for Denial
Analyzing the reason for the denial is as important as submitting it. Most denials include a reason code that explains why the claim wasn’t paid. Here are some common reasons for denials:
- Coding Errors: In this case, a claim uses incorrect ICD-10 or CPT codes.
- Medical Necessity: The insurance company believes the treatment or service wasn’t medically necessary.
- Missing Information: In this case, a patient’s details or insurance information can be missing.
- Timely Filing: If claims are filed after the insurance company’s deadline, they may be denied or rejected.
And it is the most important step to know the exact reason for denial. Because if you don’t know, you won’t be able to determine the next steps in the denial management process.
Step 4: Correcting the Claim
Once you’ve understood the reason, the next step is to correct the claim. You’ll address all the issues we mentioned above, such as adding missing information, fixing coding errors, and addressing the insurance company’s concerns about medical necessity.
Denial management in medical coding plays the most important role in this process. As coders will recheck the denied claims and correct any issues that they find. At this stage, they’ll work closely with physicians to clarify diagnoses or treatments that have been represented incorrectly.
At Providers Care Billing, LLC, we’re experts in providing denial management services. Our team of skilled coders identifies errors and fixes them quickly.
Step 5: Appealing the Denial
The next step is to appeal the denial claims. But you may be thinking How to appeal an insurance claim denial? First, it involves gathering supporting documentation and submitting a formal appeal to the insurance company. This mostly includes medical records, additional justification for the procedure, and a letter of company necessity from the healthcare provider.
This process can be time consuming, but, as you know, it is necessary to get the claims paid. Furthermore, we always suggest that the appeal should be well-documented and clearly explain why the claims should be approved.
Step 6: Tracking and Monitoring
After submission, it’s essential to track the status of the claim. Insurance companies must have a follow-up system because appeals don’t resolve on their own. And companies may take weeks or even months to process it. During this time, payers may need to contact multiple times to monitor the claim’s status.
So, denial management software is extremely helpful for this. These tools provide real time updates and make sure that all claims are properly tracked.
Step 7: Final Resolution
Now comes the point where the insurance company will either approve or deny the claim again. The first condition is that they’ll approve it and will send the reimbursement. But if it got rejected again, then healthcare providers must identify the reason. They should either appeal it again or write it off, as the company’s decision is final.
What is the Role of Revenue Cycle Denial Management, and why is it Important?
RCM denial management is a part of the broader revenue cycle management process, as it involves the entire process of patient registration, insurance verification, coding, billing, and collection.
- By incorporating denial management into the overall RCM process, a healthcare provider will be able to identify the issues earlier. So they can resolve them before they become major problems.
- It ensures that the healthcare providers receive the reimbursement that they deserve.
- Proper healthcare denial management improves their financial health and ensures claims are processed efficiently.
How Outsourcing Denial Management Services Can Help?
Outsource denial management services can be an excellent solution for all healthcare providers, because they are usually overwhelmed by the complexity of this management. It helps them to reduce administrative burden, improve their claim accuracy, and ultimately increase revenue. Professional denial management services, such as those offered by Providers Care Billing, LLC, have the expertise and tools to handle insurance claim denials.
Conclusion
Denial management workflow is the most important part of the revenue cycle that can’t be overlooked. Every step of this process, from identifying reasons to appealing claims, should be very carefully managed.
And we, Providers Care Billing, LLC, are one of the top medical billing companies in USA. We’re serving multiple healthcare providers across various states, including Arkansas, Alaska, Florida, and many more. And if you’re from one of them who are struggling with claim denials and need help with any medical billing & coding services, we’re here to assist.
Contact us today to schedule a FREE consultation and learn how our denial management workflow or medical coding services can improve your revenue cycle.
FAQs
What is denial management?
It is the process of handling insurance claim denials. It usually starts with identifying the reasons that cause denials and correcting issues, and leads to appealing claims to make sure payers are properly reimbursed.
Why is denial management in medical billing important?
Because it makes sure that providers get paid for the services they provide. Because it helps in revenue loss by addressing claims denials, which ultimately improves cash flow.
What are the most common causes of claim denials?
Incorrect coding, missing information, lack of medical necessity, and late claim submission are the most common causes of denials.
How can healthcare providers reduce claim denials?
By using accurate coding, verifying insurance, submitting clean claims on time, and regularly training staff.
What is the difference between a claim rejection and a denial?
A rejection happens before processing due to errors, while a denial happens after processing when payment is refused.